


 |
 |
|||||||
 |
||||||||
|
|
||||||||
|
|
|
|
|
|
|
|
|
|
|
E.C.P.
Hypertension |

|

|
External Counterpulsation Therapy (ECP) therapy is an exciting option for the treatment of heart disease, specifically Coronary Artery Disease. Many people who suffer from heart disease are unable to supply enough oxygen-rich blood to nourish the heart muscle (ischemia). The symptom commonly associated is angina (angina pectoris), or chest pain. Currently, many cardiologists prescribe ECP therapy for the treatment of angina. |
|
ECP has helped people throughout the world regain their quality of life. It has given new hope to many of those suffering from heart disease. After completion of ECP therapy, many people return to an active and fulfilling lifestyle.
What is ECP? ECP is a non-invasive therapy designed to improve circulation and blood flow to the heart. ECP therapy is prescribed for the treatment of Coronary Artery Disease. ECP is safe, easy, and effective. The therapy consists of 35 daily treatments lasting for one hour per day. ECP is administered on an outpatient basis and requires no hospitalization. Best of all, ECP is an exciting option for those people who have had, or are not good candidates for bypass surgery or angioplasty. If medication does not provide adequate relief from angina, ECP could be a positive alternative to invasive procedures. What does ECP do? ECP helps to alleviate symptoms of angina by increasing blood flow to the coronary arteries and heart muscle. This therapy does not remove blockages or stop the disease process. However, ECP helps revascularize the heart muscle through the development of collateral vessels. Collateral vessels help to increase blood supply to the heart muscle. Clinical Studies have shown:
|
|
How does ECP work?
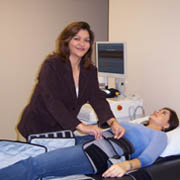
During ECP therapy, pressure cuffs are wrapped firmly around the calves, thighs, and buttocks. The cuffs inflate and deflate between each heart beat. When inflated, the cuffs squeeze blood toward the heart increasing coronary perfusion pressure, coronary blood flow and oxygen supply. This process helps oxygenated blood reach the heart muscle, further reducing or eliminating angina pain. |
|
Is ECP Painful?
No. ECP is a non-invasive procedure that does not typically cause pain. However, some patients may experience minor bruising or skin irritation as a side-effect of ECP treatment. Do insurance companies pay for ECP? Yes. Medicare will pay for ECP treatment when it is prescribed by a cardiologist. Many private insurance companies are also paying for ECP treatment. Is ECP an appropriate treatment option? ECP may be appropriate if you answer "yes" to one or more of the following questions:
|